For U.S. Healthcare Professionals
For U.S. Healthcare Professionals
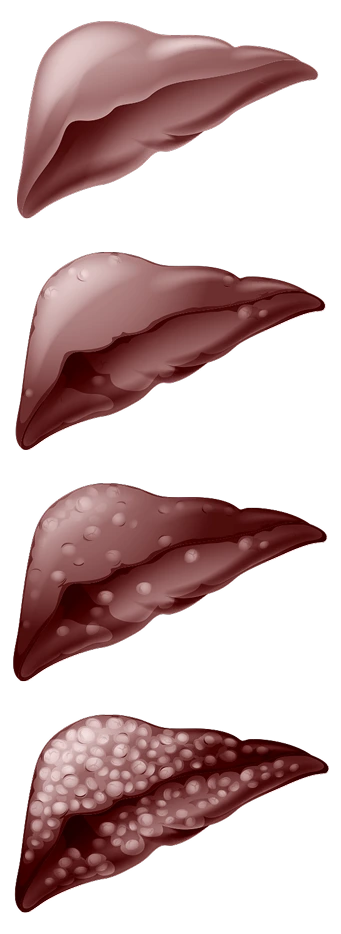
Chronic liver disease (CLD) can progress to cirrhosis and cause complications like HE,
which requires prompt attention to manage HE episodes1-3

US adults have liver disease (2018 data)6
By 2030,
adults are estimated to have cirrhosis7
Who has a high risk of MASLD/MASH? Those diagnosed with type 2 diabetes (or prediabetes), obesity (or metabolic syndrome), hepatic steatosis (on imaging), or persistently elevated liver enzymes (AST or ALT >30 IU/L for >6 months)
Who has a high risk of ALD? Those with a history of heavy alcohol use (or binge drinking), including alcohol use disorder

Medical history and physical exam alone are often insufficient to detect cirrhosis10
Up to
40%of patients with cirrhosis are asymptomatic11


Median survival
decreases from
>12
years to <2
years
after progression from
compensated to decompensated
cirrhosis1,2
Explore an enhanced learning experience about
cirrhosis and its progression
Data from a retrospective study that included patients (N=476) diagnosed with liver cirrhosis at a non-transplant hospital in Vienna from January 2015 to March 2020. Etiology of cirrhosis, sex, weight, height, presence of ascites or HE, medication, diabetes, endoscopy reports of varices, and imaging reports were assessed at baseline.9
ALD, alcohol-associated liver disease; ALT, alanine aminotransferase; AST, aspartate aminotransferase; CLD, chronic liver disease; ELF, enhanced liver fibrosis; FIB-4, fibrosis-4 index; MASH, metabolic dysfunction–associated steatohepatitis; MASLD, metabolic dysfunction–associated steatotic liver disease.
1. Garcia-Tsao G. In: Goldman L et al, eds: Goldman-Cecil Medicine. 26th ed. Elsevier; 2016:990-8.e3. 2. Poordad FF. Curr Med Res Opin. 2015;31(5):925-937. 3. Shawcross DL et al. Eur J Gastroenterol Hepatol. 2016;28(2):146-152. 4. Rinella ME et al. Hepatology. 2023;77(5):1797-1835. 5. Cusi K et al. Endocr Pract. 2022;28(5):528-562. 6. CDC, National Center for Health Statistics. Summary Health Statistics: National Health Interview Survey, 2018. Accessed December 14, 2024. https://ftp.cdc.gov/pub/Health_Statistics/NCHS/NHIS/SHS/2018_SHS_Table_A-4.pdf 7. Wong RJ et al. Clin Transl Gastroenterol. 2025;16(5):e00823. 8. Jophlin LL et al. Am J Gastroenterol. 2024;119(1):30-54. 9. Schwarz M et al. PLoS One. 2023;18(8):e0290352. 10. de Bruyn G, Graviss EA. BMC Med Inform Decis Mak. 2001;1:6. 11. Heidelbaugh JJ, Bruderly M. Am Fam Physician. 2006;74(5):756-762. 12. Liu Y et al. BMC Gastroenterol. 2025;25(1):16. 13. Bajaj JS et al. J Hepatol. 2014;60(5):940-947. 14. Wu Z et al. Front Cell Infect Microbiol. 2023;13:1218552. 15. Garcia-Tsao G et al. Hepatology. 2017;65(1):310-335. 16. Vilstrup H et al. Hepatology. 2014;60(2):715-735. 17. Sanyal AJ et al. N Engl J Med. 2021;385(17):1559-1569.